In the journey of innovative drug development, a profound understanding of how a candidate drug behaves within a biological system and the effects it produces is paramount. Pharmacokinetics (PK) and Pharmacodynamics (PD) studies form the cornerstone of this understanding. They not only reveal the Absorption, Distribution, Metabolism, and Excretion (ADME) processes of a drug but also elucidate the complex relationship between drug concentration and its effects, providing critical data to assess safety and efficacy, and optimize dosing regimens. Prisys Biotech, leveraging its deep expertise in preclinical research, particularly its leading capabilities with Non-Human Primate (NHP) models, offers high-quality PK/PD research services to global partners, accelerating the transition of new drugs from the laboratory to the clinic.
I. Pharmacokinetics (PK) Research: Mapping the Drug's Journey In Vivo
Pharmacokinetics (PK) is precisely defined as the study of what the body does to the drug, quantitatively describing the time course of drug Absorption, Distribution, Metabolism, and Excretion (ADME). Clinical Pharmacokinetics applies these fundamental principles to individual patients, aiming to optimize drug therapy regimens for personalized and precise medicine, thereby maximizing therapeutic outcomes while minimizing adverse effects.
The core objectives of PK studies include:
- Enhancing Efficacy and Reducing Toxicity: Guiding the rational design of dosage and frequency based on understanding concentration-time profiles.
- Assessing Patient Compliance: Monitoring drug concentrations can indirectly reflect adherence to prescribed medication.
- Evaluating Organ Function: Drug metabolism and excretion are closely linked to liver and kidney function; changes in PK parameters can indicate the functional status of these organs.
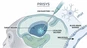
Underpinning these applications is the often strong correlation between drug concentration and its pharmacological effect. Although the drug concentration at the actual site of action (e.g., receptors in specific tissues) most directly reflects the effect, these sites are typically inaccessible for direct sampling. For instance, with digoxin, which acts on the myocardium, routinely obtaining heart tissue samples is unfeasible. Fortunately, by monitoring drug concentrations in easily accessible biological matrices like blood/plasma (the most common matrix, see Fig. 1-1), urine, or saliva, we can indirectly infer drug exposure at the site of action.

The key concept supporting this inference is Kinetic Homogeneity. It postulates that, in most cases, a predictable proportional relationship exists between drug concentrations in plasma (or blood) and those at the target tissue or receptor site (Fig. 1-2). This means changes in plasma drug concentration reflect parallel changes in tissue drug concentration. As plasma concentration increases, concentrations in most tissues rise proportionally, and vice versa (Fig. 1-3 shows a simplified illustration).


Kinetic homogeneity is a foundational assumption for clinical pharmacokinetics practice and the development of preclinical PK study models. It allows us to establish therapeutic windows (target concentration ranges) and toxicity thresholds based on readily measurable plasma concentrations. However, it's crucial to recognize that this assumption may not hold true for all drugs. Certain drugs, due to their physicochemical properties (e.g., molecular size, lipophilicity/hydrophilicity, ionization), can accumulate preferentially in specific tissues. Digoxin, for example, concentrates in the myocardium, while highly lipophilic drugs (like benzodiazepines) tend to accumulate in adipose tissue. Understanding these characteristics is vital for accurately interpreting PK data, especially when designing and evaluating preclinical PK studies, including those conducted in NHP models, where the expert team at Prisys Biotech carefully considers these factors.
II. Pharmacodynamics (PD) Research: Unveiling Drug Mechanism and Effect
Pharmacodynamics (PD) focuses on the quantitative relationship between drug concentration and the body's response, encompassing both therapeutic effects and adverse reactions, including their intensity and time course. Drug effects originate from the interaction with specific targets (e.g., receptors). These targets are widely distributed, potentially residing on neurons in the central nervous system (e.g., opioid receptors mediating analgesia), on myocardial cells (influencing contractility), or even within pathogens (e.g., antibiotics disrupting bacterial cell wall synthesis).
In simplified models, the drug concentration at the site of action directly dictates the intensity of the pharmacological effect (Fig. 1-4). However, the actual drug response is modulated by numerous factors, such as:
- The density and number of receptors on the cell surface.
- The efficiency of intracellular signal transduction pathways (second messenger systems).
- Downstream regulatory mechanisms involving gene transcription and protein synthesis.
These complex biological factors contribute to significant inter-individual variability in drug response and can lead to potentiation or tolerance to drug effects, causing response variations even within the same individual over time. This underscores the importance of conducting rigorous PD studies, particularly in models like NHPs that better mimic human physiology. The PD services offered by Prisys Biotech help clients thoroughly understand these intricate relationships.

By testing across a sufficiently wide range of concentrations, the maximum effect (Emax) can be determined. Plotting drug concentration (often logarithmically transformed) against the effect typically yields a characteristic curve (the dose-response or concentration-effect curve), revealing a threshold concentration above which the effect plateaus (Fig. 1-5).
A common metric for comparing drug potency is the Half-maximal Effective Concentration (EC50), the concentration required to achieve 50% of the Emax. When comparing two drugs, the one with the lower EC50 is considered more potent, meaning a smaller dose is needed to achieve the same level of effect.

However, EC50 solely reflects potency and doesn't fully represent a drug's clinical superiority, nor does it encompass information like the duration of effect. Duration of effect is a more complex parameter determined by factors such as drug-receptor binding kinetics and the persistence of downstream signaling.
Tolerance refers to the phenomenon where the effect of a drug diminishes with continuous administration. Tolerance can arise from PK factors (e.g., increased drug metabolism leading to lower concentrations at a given dose) or PD factors (e.g., receptor downregulation or desensitization causing a reduced effect at the same concentration). For example, patients on chronic opioid therapy for pain often require dose escalation to maintain analgesic efficacy. Tolerance can be visualized as a rightward shift in the concentration-effect curve (Fig. 1-6). Tachyphylaxis is a distinct type of tolerance characterized by rapid onset, where increasing the dose often fails to restore the effect, although it might be reversible after a drug-free interval.

Clinical Considerations and the Value of Prisys Biotech Services:
Tolerance Management: Understanding tolerance mechanisms is crucial for clinical strategies. For instance, continuous use of organic nitrates (like nitroglycerin) for angina can lead to tachyphylaxis; intermittent dosing (e.g., a "nitrate-free interval") is often employed clinically to maintain efficacy. For opioids, a balance must be struck between analgesia, tolerance, and dependence risk. Slow dose titration can sometimes allow patients to develop physiologic tolerance to certain side effects, enabling the use of higher therapeutic doses. This differs from psychological dependence (subjective craving).
Potency vs. Clinical Choice: Potency (EC50) reflects the amount of drug needed for a given effect. A more potent drug isn't necessarily "better"; it simply means a lower dose might be required. If two drugs are given at equipotent doses (doses producing the same intensity of effect), similar primary efficacy should theoretically be observed. Clinical choices involve a comprehensive assessment of efficacy, safety, convenience, cost, and other factors.
The Central Role of PK/PD in Drug Development: Integrating PK and PD characteristics through PK/PD analysis and modeling is indispensable in modern drug development. This integration helps predict effective dose ranges in humans, optimize dosing regimens, understand exposure-response relationships, and crucially supports Investigational New Drug (IND) applications.
Prisys Biotech specializes in providing high-quality preclinical PK/PD research services. We utilize advanced analytical techniques and diverse animal models, with a particular strength in Non-Human Primate (NHP) models which offer high translational relevance to humans. We deliver robust pharmacokinetic parameter determination, pharmacodynamic assessments, biomarker analysis, and PK/PD relationship studies. Our expert team is dedicated to helping clients gain deep insights into their candidate drugs, optimize development strategies, mitigate risks, and effectively support IND submissions and subsequent clinical development.

Conclusion
Pharmacokinetics (PK) and Pharmacodynamics (PD) are the twin pillars for understanding drug action, guiding rational drug use, and driving successful new drug development. Accurate and reliable PK/PD study data are fundamental for making critical development decisions.
Prisys Biotech, with its specialized knowledge and extensive experience in preclinical PK/PD research, particularly its unique advantages in utilizing NHP models, stands as your trusted partner. We are committed to providing comprehensive services, from study design to data interpretation, to help accelerate your drug development timeline.
Interested in learning more about Prisys Biotech's PK/PD research services or discussing your specific project needs? Contact us today!