Introduction: Overcoming the Blood-Brain Barrier with Direct CNS Delivery
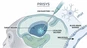
The blood-brain barrier (BBB) presents a formidable challenge for delivering therapeutics to the central nervous system (CNS). Direct CNS delivery techniques, including intrathecal (IT), intracerebroventricular (ICV), and intraparenchymal (ICM) administration, are crucial strategies to bypass this barrier. These routes enable precise drug delivery, maximize therapeutic concentrations within the CNS, and minimize peripheral exposure and associated toxicities. Consequently, direct CNS administration, particularly intrathecal injection, is increasingly utilized for advanced modalities like oligonucleotide therapies (ASOs, siRNAs) and cell and gene therapies (CGT).
Compared to systemic administration, direct CNS delivery rapidly achieves high drug concentrations within the target tissue, often obviating the need for large, potentially systemically toxic doses. This advantage allows the development of compounds that might otherwise be discontinued due to systemic toxicity profiles. Furthermore, the relatively contained circulation within the cerebrospinal fluid (CSF) and brain parenchyma, coupled with the BBB limiting efflux into systemic circulation, ensures sustained high drug levels in the CNS while minimizing systemic exposure. This reduces the risk of peripheral side effects and potentially lowers the immunogenicity risk associated with biologics, paving the way for safer and more effective treatments for debilitating CNS disorders.
This article focuses on intrathecal (IT) administration, summarizing key procedural aspects, discussing advantages and disadvantages, and highlighting potential toxicological risks encountered during non-clinical safety studies, aiming to support robust preclinical evaluation of CNS therapeutics.

J.Pers.Med.2022,12,1979
Understanding Intrathecal (IT) Injection
Intrathecal (IT) injection involves the administration of a therapeutic agent directly into the subarachnoid space, the area surrounding the spinal cord that contains CSF. This is typically achieved via lumbar puncture. Once administered, the drug disperses throughout the CSF, reaching target sites within the brain and spinal cord. Procedurally, IT delivery can be accomplished via direct lumbar puncture, catheter placement via lumbar puncture, or catheter placement via cisterna magna puncture (though less common for routine preclinical IT). Delivery systems can range from external pumps to semi-implanted or fully implanted devices for chronic administration. The lumbar puncture needle must traverse several layers: skin, supraspinous ligament, interspinous ligament, ligamentum flavum, epidural space, dura mater, subdural space, and arachnoid mater to reach the subarachnoid space.
Key Considerations for Non-Clinical IT Administration
Successful and reproducible IT administration in non-clinical species requires careful technique and species-specific knowledge:
Injection Site & Confirmation:
Non-Human Primates (NHPs) & Dogs: The lumbar region, typically between the L3/L4 or L4/L5 vertebrae, is preferred. This area corresponds to the cauda equina, minimizing the risk of direct spinal cord injury. The larger lumbar cistern volume in these species facilitates needle placement. Younger NHPs may require puncture at higher levels (L2/L3 or L3/L4). Successful placement is confirmed by the appearance of clear CSF outflow from the needle hub.
Rats & Mice: The L5/L6 intervertebral space is commonly used. A characteristic tail flick is often considered indicative of successful subarachnoid space entry.
Rabbits: The L6/L7 intervertebral space is typically targeted, with CSF outflow confirming correct placement.
Post-Injection: Following injection, maintaining needle placement for a brief period (e.g., 5-10 minutes in NHPs, potentially longer in rodents) and positioning the animal head-down (Trendelenburg position) can facilitate rostral distribution of the injectate towards the brain ventricles and limit pooling at the injection site.
Repeat Dosing Studies:
Many CNS therapies, especially oligonucleotides, require repeat IT administration. Preclinical studies must evaluate the tolerability of repeated injections and assess local irritation potential. Both the mechanical trauma of repeated punctures and the formulation/drug substance itself can contribute to local reactions. Careful monitoring of the injection site and detailed histopathological examination are critical. For example, repeat IT dosing of ziconotide has been associated with local irritation, necessitating close observation.
Advantages and Disadvantages of IT Administration
Advantages:
- Direct CNS Targeting: Bypasses the BBB, delivering drug directly to the site of action.
- High CNS Concentration: Achieves CSF drug concentrations potentially >100-fold higher than equivalent intravenous doses.
- Reduced Systemic Exposure: Minimizes peripheral side effects and toxicity.
- Lower Immunogenicity Risk: Reduced systemic exposure can lower the risk of immune responses to biologic therapies.
- Enhanced Efficacy/Lower Dose: Enables potent CNS effects at lower total doses compared to systemic routes (e.g., IT baclofen for spasticity).
- Prolonged CNS Half-Life: Drug clearance from the relatively small volume of CSF (approx. 140 mL in humans vs. 3500 mL blood) is often slower than from plasma .
Disadvantages & Risks:
Clinical:
- Procedural Complications: Post-lumbar puncture headache (PLPH), back pain, infection (meningitis), bleeding/hematoma.
- Misplacement: Accidental injection into subdural or epidural spaces (clinically reported up to 10% ).
- Patient Compliance: Repeat lumbar punctures can be poorly tolerated, impacting long-term treatment adherence. Combination IV/IT regimens are sometimes explored.
- Technical Difficulty: Challenging in infants, patients with spinal deformities, or obesity. Ultrasound or other imaging guidance may be required.
Non-Clinical (Toxicology Concerns):
- Neurotoxicity: Direct drug effects or formulation excipients can cause neuronal damage (vacuolation, necrosis), gliosis, or functional deficits. Nusinersen studies in juvenile monkeys showed transient spinal reflex deficits and neuronal changes at high doses .
- Inflammation: Chemical meningitis/encephalitis, characterized by inflammatory cell infiltrates (mononuclear cells, macrophages) in the meninges or parenchyma.
- Injection Site Reactions: Mechanical trauma and/or drug irritation can lead to spinal nerve root irritation, axonal degeneration, demyelination, gliosis, inflammation, and granuloma formation at or near the injection site.
- Increased Intracranial Pressure (ICP): Rapid injection of large volumes can acutely increase ICP, potentially causing clinical signs like nausea or vomiting (observed in animals and humans).
- Off-Target Effects: Histopathological changes may be observed distant from the injection site, e.g., brain (hemorrhage, gliosis, cellular infiltrates) or sciatic nerve (axonal/fiber degeneration).
Case Examples: Nusinersen and Tofersen
Nusinersen (Spinraza®) and Tofersen (Qalsody®) are antisense oligonucleotides (ASOs) approved for Spinal Muscular Atrophy (SMA) and a specific form of Amyotrophic Lateral Sclerosis (ALS), respectively. Both rely on IT administration for efficacy.

Nusinersen: Targets SMN2 pre-mRNA to increase functional SMN protein production, addressing the underlying cause of SMA. Motor neuron cell bodies reside primarily in the spinal cord and brainstem. IT delivery directly targets these cells. Preclinical studies in SMA mouse models demonstrated that direct CSF injection extended survival and protected motor neurons. IT administration achieves broad distribution throughout the spinal cord (highest concentrations) and brain, with prolonged tissue retention.
Toxicology Findings: Non-clinical IT studies for both drugs revealed risks such as neuronal vacuolation, neuronal/glial necrosis, and injection site inflammation (mononuclear cell/macrophage infiltration). Clinically, Nusinersen is associated with procedural risks (back pain, headache) and potential drug/class effects (thrombocytopenia, renal toxicity). Tofersen carries risks including serious neurologic events like myelitis, aseptic meningitis, and increased ICP, alongside procedural/inflammatory pain. These findings underscore the need for careful clinical monitoring, including CSF analysis, neurological exams, and potentially spinal imaging or ICP assessment, particularly given Nusinersen's use in pediatric populations where spinal anatomy is developing.
Implanted Catheters and Chronic Dosing
For therapies requiring frequent or continuous administration, implanted IT catheters connected to subcutaneous ports or pumps offer an alternative to repeated lumbar punctures. However, this approach carries surgical risks, potential for infection (including meningitis), catheter displacement or occlusion, and requires careful management. Local tissue reaction to the catheter material and the drug formulation remains a consideration, necessitating evaluation in non-clinical studies.
Conclusion: Navigating the Complexities of Preclinical IT Studies
Intrathecal injection is a powerful and increasingly essential route for delivering novel CNS therapeutics, effectively bypassing the BBB and enabling targeted treatment. However, its successful application requires careful consideration of procedural nuances across different preclinical species and a thorough understanding of potential local and systemic toxicities. Rigorous non-clinical safety assessment, including detailed evaluation of neurobehavior, neuropathology (at injection site and distal CNS regions), and potential effects on ICP, is paramount.
Expertise in designing and executing these specialized non-clinical studies, including precise IT administration techniques and comprehensive toxicological evaluation, is critical for de-risking CNS drug candidates and paving the path for successful clinical translation.