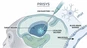
The central nervous system (CNS) comprises several compartments, including cerebrospinal fluid (CSF), brain parenchyma, ventricles, and meninges. Within the CNS, a dense network of neurons functions to transmit, store, and process information, facilitating various mental activities and controlling all behaviors in animals. Local changes in the body-such as pH fluctuations, metabolic disorders, or microbleeding-as well as peripheral circulatory changes (e.g., bacterial or viral infections) and other organ alterations (e.g., functional impairment, biological dysregulation, or inflammation) can lead to subtle shifts in the CNS microenvironment. These changes significantly affect CNS functionality, resulting in alterations in cognitive abilities, emotions, and behaviors. The brain serves as the central control system of the body, regulating all cognitive and physiological functions.
In recent years, the increasing prevalence of neurological disorders such as Alzheimer's disease, depression, schizophrenia, and Parkinson's disease has made CNS drug development a focal point in pharmaceutical research. However, high failure rates in CNS drug development are attributed to factors such as unclear disease mechanisms, the blood-brain barrier (BBB), and the irreplaceability of neurons. This article presents an overview of CNS drug screening and evaluation from the perspective of drug metabolism and pharmacokinetics (DMPK) .
Challenges in CNS Treatment
Studies of the brain's microstructure have revealed that the brain capillary bed features tight junctions between brain endothelial cells (BEC), with minimal large cell-regulating vesicles or intracellular windows. Additionally, tight junctions have been identified in the choroid plexus, confirming the existence of the blood-CSF barrier. These findings indicate that compounds entering the brain encounter at least two barriers: the BBB at the level of small arteries-capillaries-small veins and the blood-CSF barrier located in the choroid plexus. Both barriers impede the free diffusion of compounds into the CNS.
1.1 Blood-Brain Barrier (BBB)
The BBB is located between brain tissue and capillaries, presenting a significant obstacle for many drug molecules to penetrate from the circulatory system into the brain, making it the first hurdle in CNS drug development. The BBB typically manifests as a lipid membrane. Small lipophilic substances can easily enter the CNS, while many hydrophilic drugs-especially those with high charge or those that tightly bind to serum proteins-cannot cross.
The physiological characteristics of the brain include a dense capillary network beneath the cortex, approximately 650 km in length, with a vascular surface area of about 15-20 square meters. Due to this large surface area, the BBB is often considered the primary pathway for the uptake of plasma small molecules. Mature CNS endothelial cells establish the BBB to protect neural tissue from blood component fluctuations, exclude toxins, and maintain ionic homeostasis. The BBB consists of a layer of tightly packed brain capillary endothelial cells and glial cells, forming a barrier that prevents molecular transport from blood to perineuronal tissue and creates resistance to transmembrane processes. The BBB can strictly limit the entry of all compounds except for small non-polar compounds, complicating the treatment of CNS disorders.
1.2 Blood-Cerebrospinal Fluid Barrier (BCSFB)
CSF circulation begins in the ventricles via the choroid plexus and extends to the cranial side and spinal arachnoid. The BCSFB is another primary barrier; compounds from the bloodstream can directly penetrate the BCSFB or cross the BBB before reaching the CSF via diffusion or convection, regulating the entry and exit of various substances in the spinal cord. This barrier has a relatively small surface area, low diffusion rates, and rapid clearance rates, effectively preventing larger molecules, proteins, and peptides from entering.
The major transport processes within the CNS are illustrated in the accompanying figure. Brain tissue consists of interstitial fluid (ISF) and brain cells, surrounded by CSF. Scientifically, the concentration of drugs in intracellular fluid (ICF) is of primary interest (particularly its free concentration). However, current technologies cannot measure this directly. ISF serves as a theoretical indicator, and a biological barrier-the cell membrane-exists between ISF and ICF. Proteins such as albumin are present in ISF and can bind to drugs, making direct measurement challenging (though it can be inferred through microdialysis). ISF and ICF are generally considered to be in equilibrium under ideal conditions. The concentration of drugs in CSF is often regarded as approximately equal to the free drug concentration in ISF, making it a common medium for assessing brain permeability.
The BBB and BCSFB create significant barriers to the free diffusion of compounds into the CNS. The free drug concentration in plasma, in the absence of transporter-mediated transport, is thought to be approximately equal to the free concentrations in ISF and CSF.
2.1 Parameters for Evaluating BBB Permeability
Understanding the factors influencing CNS drug brain exposure and the methodologies used for evaluation is critical for drug development. Identifying key parameters for screening and optimization aims to enhance brain exposure, avoid substrates for efflux transporters, and reduce systemic clearance rates, ensuring sufficient drug reaches the target site to exert its effects. Given the challenges of crossing the BBB, selecting appropriate parameters or indicators as standards for assessment is vital.
Some common reference indicators for evaluating BBB permeability include:
2.2 Common Methods for Evaluating BBB Permeability
Due to the diverse mechanisms of small molecule permeability, common methods primarily address BBB permeability, the distribution of drugs in the brain, the concentration of free drugs in the brain, and the impact of transporters on the BBB. This section discusses commonly used methods during drug discovery.
3.1 Measurement of Free Drug Concentration in the Brain
Animal studies are the most direct and effective means to obtain drug concentrations in brain tissue, CSF, and plasma. Typically, the species used for pharmacokinetic (PK) screening should align with efficacy and toxicity. The administration route should be determined based on development goals. The procedures are similar to standard PK tests, with attention required for methods of collecting brain tissue or CSF. Test results must be calibrated against in vitro determined fu values of the compound in plasma and brain tissue, as CSF's low protein content does not necessitate correction. Kp, uu evaluates a compound's ability to penetrate the BBB, while AUCCSF and AUCp,u assess the distribution characteristics across the BCSFB, indicating whether CSF can serve as a substitute parameter for studying free drug concentrations in brain tissue.
Based on the free drug hypothesis, ideally, the free drug concentration in the brain most directly reflects the active drug concentration; however, under practical conditions, it is challenging to measure free drug concentrations in brain tissue cells. In the absence of significant transporter effects, free drug concentrations in plasma, CSF, or interstitial fluid of brain tissue serve as substitute parameters.
3.1.1 Brain Tissue Distribution Measurement
Single or multiple sampling points are used to calculate Kp,brain:

Kp,brain is relatively easy to obtain, but this parameter may introduce bias regarding compound understanding. Due to differences in the free fraction of compounds in plasma and brain tissue, compounds with a high blood-to-plasma ratio may not have high free concentrations in the brain; conversely, compounds with a lower blood-to-plasma ratio may be superior candidates. Thus, this parameter can only roughly exclude compounds with very low total brain concentrations, making it unsuitable for selecting optimal candidates.
3.1.2 Brain-Plasma Free Drug Ratio Method
Kp, uu represents the brain-plasma free drug ratio, a key parameter for evaluating the distribution equilibrium of compounds between blood and brain. It comprehensively reflects passive diffusion and transporter actions.

The free fractions in plasma and brain tissue are primarily used to convert standard PK parameters into free drug parameters. Looking at it in isolation, a higher free drug fraction generally indicates a higher effective drug concentration. However, from a holistic perspective, increased free drug fractions in plasma may lead to enhanced metabolism or excretion rates, while elevated free drug fractions in brain tissue could hinder passive diffusion into the brain. Consequently, fu cannot usually serve as a primary parameter for optimization, and its value is not inherently linked to drug efficacy.
When Kp, uu approaches 1, it reflects ideal compound characteristics, indicating good permeability and non-substrate for transporters; under these conditions, plasma free drug concentration can serve as a substitute indicator. Conversely, when Kp, uu is significantly less than 1, it suggests the compound may be a substrate for transporters or have poor permeability, necessitating structural modifications to improve compound characteristics. When Kp, uu exceeds 1, it may indicate the involvement of active transporters in transmembrane transport processes.
3.1.3 CSF Measurement Method
The concentration of drugs in CSF is often considered approximately equal to the free drug concentration in ISF, making it a common matrix for assessing brain permeability. Generally, protein concentrations in CSF are negligible. Detecting CSF concentrations in vivo poses technical challenges, primarily due to limited sampling volumes (e.g., a rat's total CSF circulation is only 250 μL), susceptibility to blood contamination during collection, and typically low concentrations (only free drug concentrations).
3.2 Blood-Brain Barrier Permeability
3.2.1 Artificial Membrane Technology
The PAMPA model employs a "sandwich" structure: a donor buffer containing the test substance at the bottom, an artificial lipid membrane in the middle, and a receptor buffer above. This model uses an artificial lipid membrane lacking transport proteins, suitable for evaluating drugs with passive diffusion mechanisms but unable to accurately predict those reliant on active transport. As most compounds enter brain tissue through passive diffusion, BBB passive permeability is critical in drug design. A high-throughput PAMPA-BBB model has been developed to assess a drug's passive permeability across the BBB.
3.2.2 In Situ Brain Perfusion Method
The gold standard for evaluating BBB permeability is the in situ brain perfusion method; however, due to its technical demands and feasibility challenges, it is seldom used for compound screening. Currently, the most common approach involves homogenizing plasma and brain tissue and applying equilibrium dialysis for measurement. For compounds with significant non-specific binding to high protein levels, the experimental equilibrium time may need adjustment to ensure true equilibrium, thus avoiding result discrepancies. Alternative methods include Transil or stepwise equilibrium dialysis. Studies have found that brain tissue binding rates are independent of species and brain tissue region, allowing human brain tissue binding rates to be derived from single species data. Additional methods include ultracentrifugation, microdialysis, and brain tissue sectioning.
3.3 P-glycoprotein (Pgp) Efflux Transport Activity
To better simulate the BBB and evaluate the permeability of test compounds across the BBB, brain-derived or non-brain-derived cell models (MDCK cell model, MDCK-MDR1 cell model, Caco-2 cell model) have been developed. Compared to PAMPA-BBB methods, cell models are more suited for studying BBB transporters. Assessing whether a compound is a substrate for Pgp and whether it undergoes efflux is crucial, as Pgp remains a significant transporter preventing drugs from entering the brain. Screening for Pgp efflux activity is vital for CNS therapy. The MDCK-MDR1 or Caco-2 cell models can assess Pgp efflux activity and guide structural modifications to overcome Pgp-mediated efflux and enhance permeability.
Prisys Biotech has an experienced DMPK team that has established in vivo PK and in vitro ADMET-related experiments for preclinical stages of new drug development, including pharmacokinetic studies in cyno macaques, acute toxicity tests, and toxicokinetics. We support the use of multiple solvents, various administration routes, and diverse tissue sampling methods. Prisys Biotech offers customized in vivo and in vitro experiments, providing superior pharmacokinetic services to assist in new drug development.